NCATS Research Team Identifies Possible Treatment for Niemann-Pick Type C1
Translational research is a team sport. To help streamline the scientific process, NIH's NCATS facilitates team-based collaborations among researchers who have varied areas of expertise.
One such collaboration includes government, academic scientists, the pharmaceutical industry and patient support groups dedicated to finding potential treatments for a rare disease known as Niemann-Pick type C1. The disease causes lipids such as cholesterol to accumulate primarily in the cells of the brain, impairing movement and leading to seizures, dementia and slurred speech, among other symptoms. The majority of patients die in their teenage years.
The Niemann-Pick type C1 research team, which includes scientists from the NCATS Division of Preclinical Innovation, recently showed that patient skin cells treated with a form of vitamin E, called delta-tocopherol, had lower accumulation of cholesterol. The team’s findings, published in the Nov. 16, 2013, issue of the Journal of Biological Chemistry, represent another potential ingredient in a treatment cocktail for Niemann-Pick type C1.
"The Niemann-Pick type C1 research collaboration is a great illustration of the NCATS approach, which combines individual initiative and teamwork to deliver results that no one group can do alone," said Christopher Austin, M.D., director of NCATS.
The Niemann-Pick type C1 team includes scientists from NCATS, the Eunice Kennedy Shriver National Institute of Child Health and Human Development and the National Human Genome Research Institute. In addition, there are academic collaborators from Washington University in St. Louis, Albert Einstein College of Medicine in New York City and University of Pennsylvania in Philadelphia as well as a pharmaceutical industry partner, Janssen Research & Development, LLC. The academic partners are funded through the Support Of Accelerated Research (SOAR), which was established by patients and their parents to find a cure for Niemann-Pick disease. The Ara Parseghian Medical Research Foundation contributed funding as well.
The collaboration began in 2008. Each team member brings a set of skills, knowledge and expertise that contributes significantly to the project, from cell biology to physiology to NCATS’ extensive drug discovery and preclinical drug development capabilities.
The group’s first step was to create an biological assay (or testing system) for Niemann-Pick type C1. The assay was screened against the NCATS Pharmaceutical Collection, which at the time included about 2,800 approved drugs, to identify drugs that had activity in Niemann-Pick type C1 cells. The hits included delta-tocopherol and cyclodextrin. The research team continued to develop cyclodextrin through NCATS' Therapeutics for Rare and Neglected Diseases (TRND) program, and the potential treatment is now undergoing evaluation in clinical trials.
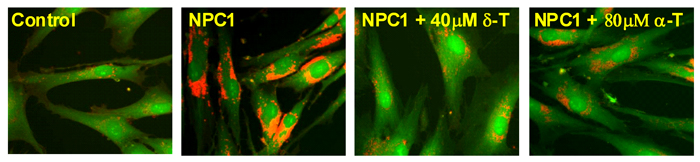
From left to right: a healthy control cell, an NPC cell, an NPC cell treated with delta-tocopherol and an NPC cell treated with alpha-tocopherol. The image shows that treatment of NPC cells with delta-tocopherol alleviates the disease characteristics in the NPC cell.
"At first, we did not pursue delta-tocopherol because of our focus on developing cyclodextrin, which looks quite promising as a potential treatment for Niemann-Pick type C1," said Wei Zheng, Ph.D., TRND biology lead and co-author of the delta-tocopherol paper. "Eventually, we followed up on delta-tocopherol and found it has a profound effect on Niemann-Pick cells and had some potential to be developed as a possible treatment."
The researchers treated skin cells with delta-tocopherol and observed that it seemed to clean up lipids that had accumulated in the cells via a process called lysosomal exocytosis, which helps cells export unwanted materials.
They also tested the alpha form of vitamin E, commonly sold in stores, and found that although it too helped reduce cholesterol and lipids in the cells, it had a much weaker effect than delta-tocopherol.
As the research continued, the team found that delta-tocopherol treatment produced similar results in cells of other lysosomal storage diseases, such as Batten, Fabry, Farber, Niemann Pick type A, Sanfillipo type B, Tay-Sachs and Wolman diseases. The unique effect and mechanism of delta-tocopherol on Niemann-Pick and the other lysosomal storage diseases reveals a new direction of future drug development for a class of drugs that target lysosomal exocytosis.
Not much is known about the mechanism by which vitamin E works, although the antioxidant effect has been extensively reported. The researchers found a clue when looking at previous findings suggesting that Niemann-Pick type C1 is associated with reduced calcium levels in lysosomes, an organelle in cells that breaks down waste materials. According to study authors, an increase in calcium in cells triggers a variety of cellular responses that reduces lipid accumulation in a disease model.
"The researchers tested this idea and found that delta-tocopherol indeed stimulated a calcium response in the Niemann-Pick cells, which enhanced lysosomal exocytosis," said John McKew, Ph.D., acting director of NCATS’ Division of Preclinical Innovation. "This knowledge is important for understanding Niemann-Pick disease and also may be valuable for studying the benefits of vitamin E."
Researchers have a lot of work to do before delta-tocopherol can be considered as a viable treatment candidate for lysosomal storage diseases. For instance, the researchers know that delta-tocopherol is metabolized quickly and does not penetrate the blood-brain barrier at a concentration at which its therapeutic effects are needed.
To address this obstacle, NCATS chemists have modified the delta-tocopherol molecule to increase its concentration in the blood stream and its ability to penetrate the blood-brain barrier. Improvements of these properties are crucial for the development of the next generation of compounds for treatment of Niemann-Pick type C1.
"The important thing about the delta-tocopherol project is that the team did not give up on it, and the molecule is showing great promise again," said Jonathan Jacoby, a rare disease advocate who has been following the team's progress. "I'm optimistic [about finding an NPC treatment] because there is a real pipeline of potential therapies as a result of this collaboration."
Posted February 2013


