Meet Chip: Brain
The brain is part of the body’s nervous system, which also includes all the nerves and the spinal cord. The blood–brain barrier allows water, gases, sugars and some other compounds to cross from the blood circulation into the fluid surrounding the brain. At the same time, the membrane blocks many potentially harmful toxins and germs. The barrier’s dual purpose can make it difficult to treat brain conditions because some potential treatments can’t cross through the barrier, and researchers are challenged by the lack of methods to predict which drugs can get through.
Scientists also need more information about brain development — the processes that generate, shape and reshape the brain, from the earliest stages of the embryo to the final years of life. Progress in finding new treatments for various diseases has been hampered by a lack of data on how potential therapeutics affect development of the brain.
Scientists could benefit greatly from having access to laboratory devices that enable them to study brain tissue, the developing brain and the blood–brain barrier. Some NIH-funded investigators have focused their research on developing such devices, with the aim to accelerate the process for testing and approving new drugs and, ultimately, get more treatments to more patients more quickly.
When the precursor cells are added to the other types of brain cells in the chip, they transform into another type of brain cells called microglia, as shown in this video.
Brain Development on a Chip
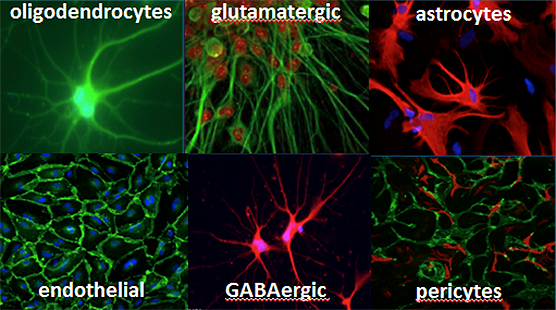
NIH-supported scientists at the Morgridge Institute for Research in Wisconsin are developing a brain on a chip with human brain tissue. The scientists generated multiple types of brain cells from a single stem cell source. Stem cells have the remarkable potential to develop into many different cell types. Stem cells are important during early life and for embryonic growth; in adults, stem cells function in tissue repair and maintenance. When these brain cells are added together in a nutrient-rich framework, they form complex, layered tissue, complete with nerve structures and blood vessels.
The scientists’ goal is to use the model to predict the effects of potential toxins on brain development. By doing initial testing in a laboratory setting with human tissue, the scientists may be able to predict potential toxic compounds on the brain with greater accuracy than current testing methods allow.
Blood-Brain Barrier on a Chip
With NIH support, a research team at Vanderbilt University is bioengineering a device that scientists could use to test compounds for their ability to cross the blood–brain barrier. The researchers used stem cell technology to generate brain tissue and blood vessels for the device. They generated brain cells and blood vessels from induced pluripotent stem cells (iPSCs) derived from adult donor cells.
iPSCs can develop into various types of brain cells and organize themselves into layers, complete with nerves and blood vessels. Other iPSCs develop into cells that form tiny blood vessels. On the chip, the brain cells and blood vessels are separated by a membrane that acts like the blood–brain barrier.
Looking Ahead
Scientists will use the bioengineered models of the brain and the blood-brain barrier to test experimental drugs. This research should provide data to accelerate the drug approval process and make new treatments available sooner to patients. Using the bioengineered systems, scientists not only could develop new treatments for brain diseases but also could more accurately predict the neurologic effects of drugs designed to treat other diseases.
In the future, researchers plan to link the brain and blood-brain barrier models with chips based on other human organs. Doing so will contribute to our knowledge about the “downstream” effects of experimental brain treatments on other organs. Quite possibly, the processing of drugs by other organs of the body (e.g., the liver) could affect the ability of drugs to cross the blood-brain barrier and also provide crucial information for scientists working to develop new and more effective treatments.