Meet Chip: Gastrointestinal System
Digestion breaks down food and liquids into nutrients — carbohydrates, protein, fats and vitamins — used by the body for energy, growth and cell repair. Parts of the nervous, immune and circulatory systems, as well as hormones and enzymes, play roles in digestion. Muscular contractions transport food and waste through the gastrointestinal (GI) system by a process called gut motility, or peristalsis. Bacteria in the GI tract, which make up the gut microbiome, also are important in digestion and in overall health. The gut microbiome makes vitamin K, which is critical for blood clotting.
Because many drugs are taken by mouth, they can affect the structure and function of the GI tract and the delicate balance of the microbiome. Although the GI lining serves as a barrier against infection, the system is sensitive to toxins, certain diseases and medicines. In addition, statistics show that problems with the nerves and muscles of the GI system affect up to 25 percent of the U.S. population, but few treatments are available to help.
Having an experimental device to study the GI system could help scientists find new treatments for GI motility problems and predict side effects of drugs on the gut and its microbiome. That is the aim of an NIH-funded project to develop a bioengineered gut on a chip.
Kidney on a Chip
NIH-supported researchers at Cincinnati Children’s Hospital and Johns Hopkins University are working on miniature systems composed of human intestinal tissue containing smooth muscle and nerves. To create these systems, the researchers have either used intestinal tissue discarded after surgery or generated induced pluripotent stem cells (iPSCs) from adult cells. Stem cells have the remarkable potential to develop into many different cell types. Stem cells are important during early life and for embryonic growth; in adults, stem cells function in tissue repair and maintenance. iPSCs can produce an unlimited supply of donor cells capable of forming GI and other types of tissues for the chip devices.
This model is a major advance because it consists not only of gut tissue but also of nerves that stimulate the action of smooth muscle that controls gut motility. The research has resulted in an experimental device that closely resembles the function of the human GI system. Scientists can use this device to study gut motility, screen potential treatments for gut motility diseases, monitor drug absorption from the gut into the bloodstream and test drugs for toxic effects on the GI system.
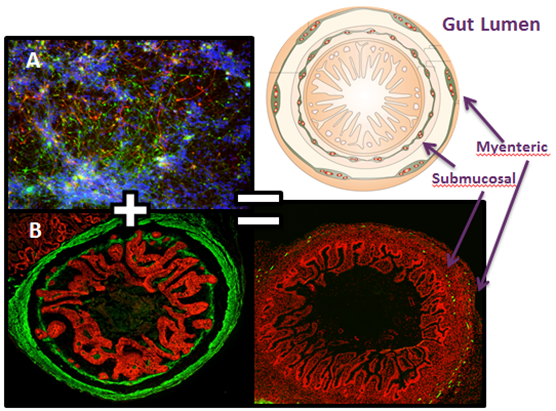
A team of researchers at Johns Hopkins University showed that the “micro-gut” (shown in red in the video) can secrete a digestive enzyme (green) in a way that mimics the function of the human GI system.
Looking Ahead
NIH-supported researchers have shown that iPSC technology or discarded surgical specimens can be used to generate a gut on a chip, complete with smooth muscle and nerve fibers. Researchers can use the device to learn more about gut motility diseases and to test experimental drugs. In addition, researchers might be able to gather data to accelerate the drug approval process and to make new treatments available sooner to patients.
Scientists also look forward to having an experimental system to learn more about the gut microbiome. Plans are in the works to link the gut on a chip with other tissue chips based on the liver and kidney to get a more complete picture of how drugs are processed in the body and to better predict their toxic effects.